Chronic Diseases - The Effects Of Autoimmune Disease And Mitochondrial Dysfunction
Chronic diseases involving the autoimmune process and abnormal immune responses are linked to mitochondrial disease. This has led to concerns being expressed about potentially irreversible processes that are connected to multiple organ disease syndrome, NAFLD, obesity, diabetes, and neurodegenerative diseases.
Author:Suleman ShahReviewer:Han JuJul 18, 202323.1K Shares445.3K Views

Chronic diseasesinvolving the autoimmune process and abnormal immune responses are linked to mitochondrial disease.
This has led to concerns being expressed about potentially irreversible processes that are connected to multiple organ disease syndrome, NAFLD, obesity, diabetes, and neurodegenerative diseases.
Loss of function in mitochondria, the key organelle for cellular energy production, can cause fatigue and other chronic disease symptoms.
Mitochondrial dysfunction and impaired bioenergetics are implicated in the pathogenesis of many chronic diseases, mainly neuroimmune or autoimmune.
Mitochondrial dysfunction, characterized by a loss of efficiency in the electron transport chain and reduced ATP synthesis, is a hallmark of aging and chronic diseases.
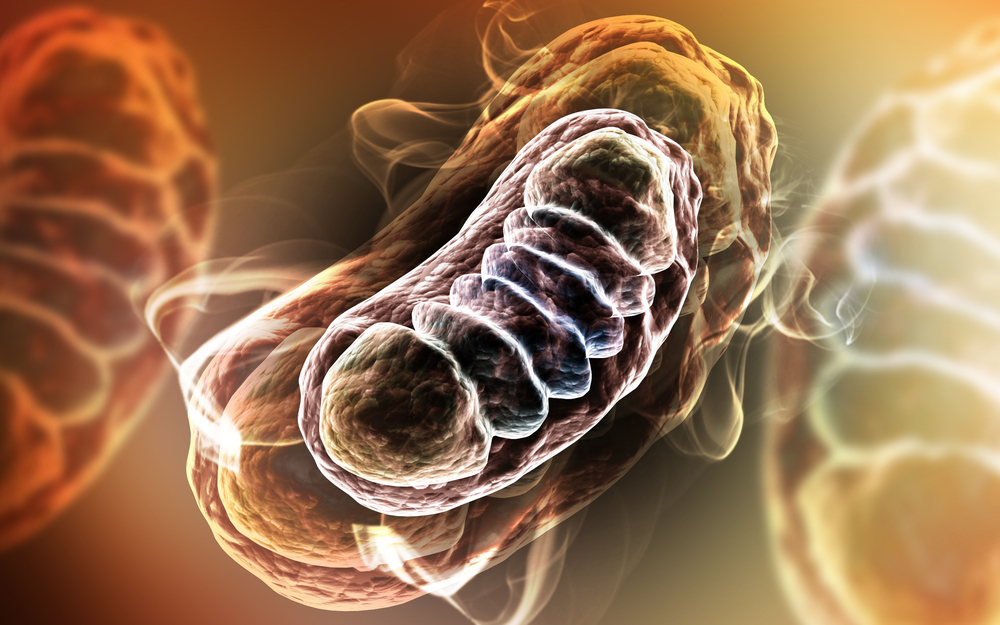
What Are Mitochondria?
The mitochondria are often referred to as the "energy factory" of the cell. Nearly every cell in the body contains a number of mitochondria, typically in the range of several thousand. They are responsible for the processing of oxygen and the conversion of substances derived from the food we eat into usable forms of energy. Mitochondria are responsible for the production of 90% of the energy that is required for our body to function.
What Are Mitochondrial Diseases?
Chronic (long-term), genetic, and frequently inherited disorders called mitochondrial diseases take place when mitochondria are unable to produce enough energy for the body to function normally. Although they can develop at any age, mitochondrial diseases can be present at birth.
Nearly every organ in the body, including the brain, nerves, muscles, kidneys, heart, liver, eyes, ears, and pancreas, can be impacted by mitochondrial diseases.
When the mitochondria don't function as well as they should because of another illness or condition, mitochondrial dysfunction occurs. There are numerous conditions that can cause secondary mitochondrial dysfunction and influence other illnesses, including:
- Cancer
- Diabetes
- Lou Gehrig’s disease
- Muscular dystrophy
- Alzheimer’s disease
Secondary mitochondrial dysfunction patients don't have primary genetic mitochondrial disease, so they don't need to worry about their symptoms escalating or getting worse.
What Causes Mitochondrial Disease?
The majority of the time, primary mitochondrial disease is a genetic disorder that can be inherited (transmitted from one set of parents to another) in a number of different ways.
Learning more about genes and DNA is useful for comprehending different inheritance types. Our characteristics, such as brown eyes or blue eyes, are inherited through our genes. DNA, the genetic "blueprint" that determines each individual's characteristics, is found in genes.
Normally, a child receives two genes from each parent—one from the mother and one from the father. A healthy set of genes are NOT passed down from the parents to a child with mitochondrial disease. The gene has changed, or mutated, which means it has become flawed. The likelihood of passing on a mitochondrial disease or diseases to future offspring can be predicted by understanding how the disease has been inherited.
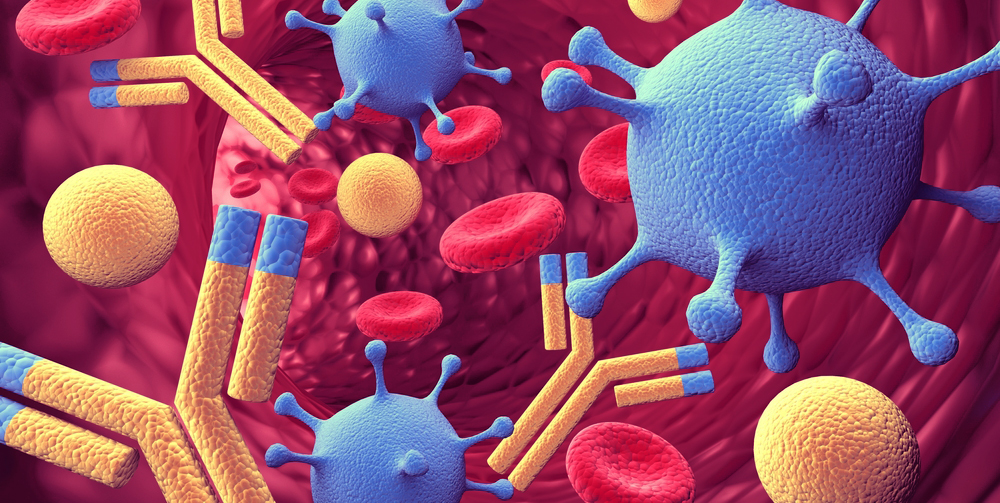
What Is Autoimmune Disease?
Diseases that are caused by the immune systemattacking healthy parts of the body are known as autoimmune diseases. Inflammationresults from this, and inflammation can set off common symptoms of autoimmune diseases such as pain, rashes, and swelling.
There are numerous autoimmune diseases. Even though they have some similar symptoms, they differ in certain ways.
What Are The Common Signs And Symptoms Of Autoimmune Disease?
The primary factor that brings on the symptoms of autoimmune diseases is inflammation, which can result in the destruction of both tissue and organs.
The following is a list of signs and symptoms that are typical of most autoimmune diseases:
- Numbness and tingling in the hands and feet
- Trouble concentrating
- Recurring low-grade fever
- Swollen glands
- Stomach ache
- Skin rashes
- Pain and swelling in the muscles, connective tissues, and/or joints
- Fatigue
Symptoms can vary in their degree of severity. Flare-ups are times when symptoms get worse, whereas remission is a period of little to no symptom activity.
Effects Of Autoimmune Disease And Mitochondrial Dysfunction In Chronic Disease
Anti-aging genes such as Klotho, FOXO 3a, p66shc, and Sirtuin 1 (Sirt 1) are linked to chronic diseases. Repression of Sirt 1 is involved with the transcriptional dysregulation of other anti-aging genes (Klotho, p66shc, FOXO1/FOXO3a) that leads to abnormal glucose, lipid, and amyloid-beta metabolism associated with programmed cell death in various cells and tissues. Anti-aging genes and their links to autoimmune and chronic diseases are relevant to irreversible programmed cell death in many tissues. Dietary effects with Sirt 1 downregulation accelerate disease progression in global communities with auto-immune diseases.
Mitophagy is a concern in chronic diseases with accelerated mitochondrial apoptosis linked to Sirt 1. Sirt 1 is involved in mitochondrial biogenesis, and its connections to other anti-aging genes via p53 deacetylation are important for mitochondrial biogenesis versus apoptosis. p53 maintains the immune system and its mitochondrial function is linked to anti-aging genes. Sirt 1 is now linked to autoimmune disease, and its regulation of p53 and anti-aging genes may be the primary defect with irreversible consequences to cell biology and programmed cell death in developing and developed countries.
Plasma heat shock protein (HSP) analysis is now essential to avoid uncontrolled immune reactions linked to Sirt 1 repression, which controls HSP metabolism. In normal aging, HSP accumulates with autoimmune reactions and mitophagy, causing age-related diseases. Abnormal core body temperature is a major concern for the early origins of chronic disease. The anti-aging gene Sirt 1 regulates core body temperature and the immune system. In chronic diseases, irreversible HSP-mediated programmed cell death should be avoided by maintaining the suprachiasmatic nucleus in the brain, which regulates core body temperature and is linked to peripheral organ disease. Sirt 1 is defective with increased HSP levels involved in autoimmune disease and mitophagy linked to irreversible programmed cell death in many organ diseases in global populations. Anti-aging genes and their connections to autoimmune disease mitophagy now identify Sirt1 as being defective with increased HSP levels involved in autoimmune disease and mitophagy connected to irreversible programmed cell death in many organ diseases in global populations.
People Also Ask
Is Depression A Chronic Disease?
Over the past few decades, theory and research on depression have increasingly focused on the recurrent and chronic nature of the disorder. These recurrent and chronic forms of depression are extremely important to study, as they may account for the bulk of the burden associated with the disorder.
What Causes Chronic Disease?
Most chronic diseases are caused by key risk behaviors: Tobacco use and exposure to secondhand smoke. Poor nutrition, including diets low in fruits and vegetables and high in sodium and saturated fats. Physical inactivity.
What Is The Difference Between Chronic Disease And Chronic Illness?
Chronic disease is defined on the basis of the biomedical disease classification, and includes diabetes, asthma, and depression. Chronic illness is the personal experience of living with the affliction that often accompanies chronic disease.
Is Anxiety A Chronic Disease?
Clinical and epidemiological data suggest that generalized anxietydisorder (GAD) is a chronic illness causing patients to suffer for many years leading to significant distress in daily lifefunctioning.
Conclusion
It is essential for naturopathic physicians to address the fundamental reasons behind chronic diseases that are associated with the autoimmune process, as the prevalence of autoimmune disorders is expected to continue its upward trend. The findings of this study make it abundantly clear that further research is required into the feasibility of adopting a multifaceted strategy for combating autoimmunity that incorporates mitochondrial support in addition to general inflammatory support.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles