Ventricular Depolarization – Role In Cardiac Function
Ventricular depolarization is capable of transferring electrical impulses into the ventricle without using the AV-His Purkinje conduction system.
Author:Suleman ShahReviewer:Han JuJul 08, 202215 Shares425 Views
Ventricular depolarizationis partially facilitated by an auxiliary pathway that connects the atrial and ventricle and is therefore capable of transferring electrical impulses into the ventricle without using the AV-His Purkinje conduction system. The ventricular depolarization process is separated into two stages: interventricular septum stimulation and simultaneous left and right ventricular stimulation.
Ventricular Depolarization And Mean Electrical Axis
The mean electrical axis is the average of all the instantaneous mean electrical vectors that occur consecutively during ventricular depolarization. During ventricular activation, impulses are initially routed down the left and right bundle branches on each side of the septum. As a result, the septum depolarizes from left to right.
Because each limb lead will "see" the series of depolarization vectors from a different viewpoint, the form of the QRS complex varies (see axial reference system).
The animated picture to the right depicts the appearance of the QRS complex for leads aVF and aVL. These two leads' positive electrodes are at +90° and - 30°, respectively.
The mean electrical axis in this image is around +45°. It is worth noting that aVF has a substantial net positive QRS. Because septal depolarization is not directed away from the lead, there is no Q wave.
Because early ventricular depolarization is mainly focused on this lead, the R wave is quite positive. Because the final depolarization of the top wall of the left ventricle is directed away from aVF, the S wave is also present. aVL, on the other hand, has an early Q wave (septal depolarization is directed away from the lead) followed by a somewhat positive R wave.
The mean electrical axis summarizes all the mean electrical vectors that occur during ventricular depolarization.
A green arrow represents the mean electrical axis in the picture to the right, which displays the identical instantaneous mean vectors as at the top of this page but overlaid on the axial reference system.
The mean electrical axis in this sample is roughly +40°. The heart's mean electrical axis is generally between - 30 and +90°. A left axis deviation is less than - 30°, and a right axis deviation is more than +90°.
Axis deviations may result from increased cardiac muscle mass (e.g., left ventricular hypertrophy), alterations in the order of ventricular activation (e.g., conduction abnormalities), or ventricular areas that are unable to be activated (e.g., infarcted tissue).
Ventricular Depolarization QRS Complex
The QRS complex consists of the Q, R, and S waves. These three waves happen in quick succession. The QRS complex denotes ventricular depolarization by representing the electrical impulse as it passes across the ventricles. The QRS complex, like the P wave, begins before ventricular contraction.
Understanding that not every QRS complex has Q, R, and S waves is critical. According to tradition, the Q wave is always negative, while the R wave is the complex's first positive wave. The QRS complex is an R wave if it solely has an upward (positive) deflection. After an R wave, the S wave is the first negative deflection.
The QRS complex will last between 0.06 and 0.10 seconds in an adult patient under typical conditions. In leads, I, aVL, V5, V6, II, III, and aVF, the QRS complex is frequently positive. In lead aVR, V1, and V2, the QRS complex is often negative.
The J-point is the intersection of the QRS complex with the ST segment. It might also be regarded as the beginning of the ST section. The J-point (also known as the Junction) is significant because it may be utilized to detect an ST-segment elevation myocardial infarction. A STEMI is diagnosed when the J-point increases at least 2 mm above baseline.
Ventricular Depolarization Vs Repolarization
The ventricular depolarization process is separated into two stages: interventricular septum stimulation (shown by a small arrow pointing through the septum into the right ventricle) and simultaneous left and right ventricular stimulation (represented by a larger arrow pointing through the left ventricle and toward the left side of the chest).
Ventricular Depolarization ECG
ECG Morphology
A positive-going deflection will arise if a wavefront of depolarization travels towards the electrode connected to the + input terminal of the ECG amplifier and away from the electrode linked to the - terminal. A negative-going deflection will be noticed when the waveform travels from the + electrode to the - electrode.
If the waveform moves perpendicular to the line connecting the two electrode locations, no deflection or a biphasic deflection is generated.
Thus, the voltage recorded along a specific lead axis (the vector connecting the - to the + electrode) at a particular time is determined by projecting the vector reflecting the amount and direction of depolarization onto that axis.
As a consequence, when the lead axis in the picture above points from left to right, parallel to the direction of depolarization movement, a positive-going complex arises. When the two directions are anti-parallel, a negative-going complex is formed.
The above ideas may be used to establish how the ECG waveforms emerge at each moment. For example, since the direction of atrial depolarization is almost parallel to the axis of lead II (from RA to LL), a positive-going deflection (P wave) would arise in that lead.
Because the ventricular muscle in the left ventricle is thicker than in the right, the summated depolarization of the two ventricles is downward and toward the left leg, resulting in a positive-going deflection (R-wave) in lead II because the depolarization vector is in the same direction as the lead II axis.
As septal depolarization proceeds from left to right, the depolarization vector is directed towards the - electrode of lead II (RA), resulting in a negative-going deflection (Q-wave).
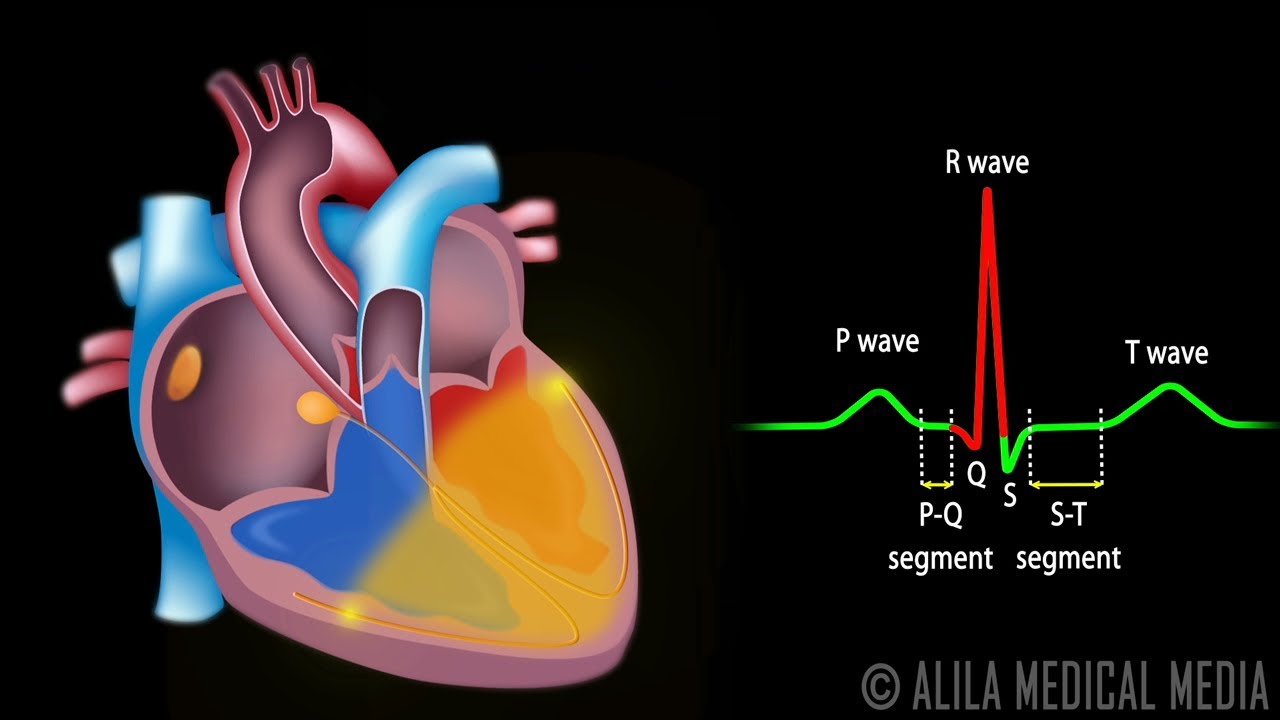
Cardiac Conduction System and Understanding ECG, Animation.
Heart Activation During ECG
The following are the major phases of cardiac activation when the ECG is recorded in the lead II.
- The sino-atrial node is the source of the heart's electrical activity. The impulse then swiftly travels to the atrioventricular node through the right atrium. It also extends straight from the right atrium via the atrial muscle. The P-wave is produced by activating the muscles in both atria.
- The impulse goes slowly via the AV node, swiftly through the His bundle, then through the bundle branches, the Purkinje network, and lastly into the ventricular muscle.
- The interventricular septum, which activates fro activates from left to right, and the ventricular muscle to be engaged. This produces the Q-wave.
- The left and right ventricular free walls, which comprise most of the muscle in both ventricles, are recruited. The endocardial surface is activated first, followed by the epicardial surface. This produces the R-wave.
- At a later stage, a few tiny portions of the ventricles are activated. This produces the S-wave.
- The ventricular muscle finally repolarizes. This produces the T-wave.
Cardiac Axis
The cardiac axis is the mean direction of the frontal plane wave of ventricular depolarization evaluated from a zero reference point. The mean QRS axis is calculated by measuring the heights of the QRS waves in the three leads.
Ventricular Repolarization T Waves
The T wave is an indication of ventricular repolarization. In general, the T wave has a positive deflection.
The explanation is that the last cells in the ventricles to depolarize are the first to repolarize. This happens because the final cells to depolarize are in the ventricle's subepicardial area, and these cells have shorter action potentials than cells in the ventricular wall's subendocardial regions.
Although the subepicardial cells depolarize after the subendocardial cells, the subepicardial cells repolarize in phase 3 before the subendocardial cells.
Repolarization waves are therefore usually oriented in the opposite direction as depolarization waves, and repolarization waves traveling away from a positive recording electrode create a positive voltage.
The T wave lasts longer than the QRS complex, which signifies depolarization. The extended length arises because repolarization wave conduction is slower than depolarization wave conduction. This is because the repolarization wave does not use the high-velocity bundle branch and purkinje system, relying instead on cell-to-cell conduction.
Following the T wave, a minor positive U wave may be noticed. This wave is the final vestige of ventricular repolarization. Inverted T waves or strong U waves imply underlying disease or repolarization-related disorders.
QT Interval For Ventricular Depolarization And Repolarization
The QT interval indicates the time required for both ventricular depolarization and repolarization, approximating the average ventricular action potential length. This period may vary from 0.20 to 0.40 seconds, depending on heart rate.
At high heart rates, the length of ventricular action potentials shortens, reducing the QT interval. Because extended QT intervals might indicate vulnerability to certain forms of tachyarrhythmias, it is critical to assess if a specific QT interval is abnormally lengthy.
In practice, the QT interval is represented as a "corrected QT (QTc)," which is calculated by dividing the QT interval by the square root of the R-R interval (interval between ventricular depolarizations). This enables a measurement of the QT interval that is not affected by heart rate. Regular adjusted Q-c intervals are fewer than 0.44 seconds.
As it happens during ventricular depolarization, there is no discernible wave signifying atrial repolarization on the ECG. The atrial repolarization wave is tiny in amplitude (i.e., low in voltage), and the much bigger ventricular-generated QRS complex obscures it.
People Also Ask
What Is Ventricular Depolarization And Repolarization?
The QRS complex represents ventricular depolarization and activation. In contrast, ventricular repolarization is the period between the start of the QRS complex and the conclusion of the T wave (QT interval). Ventricular repolarization is a sophisticated electrical phenomenon that has been extensively researched.
What Happens During Depolarization Of The Heart?
Because depolarization of the heart causes contraction of the heart muscles, an EKG provides an indirect indication of heart muscle contraction. Without external stimulation, the cardiac cells will depolarize. Automaticity, or autorhythmicity, is a feature of heart muscle tissue.
When Do Ventricles Depolarize?
The isoelectric phase (ST-segment) that follows the QRS and ends at the start of the T wave is when both ventricles are depolarized. This section corresponds closely to the plateau period of ventricular action potentials.
What Is Atrial And Ventricular Depolarization?
The P wave indicates atrial depolarization, the QRS complex reflects ventricular depolarization, and the T wave reflects ventricular repolarization, as seen in Figure 6.10. Because it overlaps with the much bigger QRS complex, atrial repolarization cannot typically be distinguished from the ECG.
Conclusion
When at rest, heart muscle cells are polarized. On the skin surface, depolarization and repolarization of the whole heart may be monitored. An ECG is a kind of measurement. The contraction of the cardiac muscles occurs as the heart depolarizes. Without external stimulation, the cardiac cells will depolarize. Automaticity, or autorhythmicity, is a feature of heart muscle tissue. The cells that originate and spread the contract signal are part of the heart's conducting system, a network of specialized cardiac muscle cells that generate and distribute electrical impulses.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles