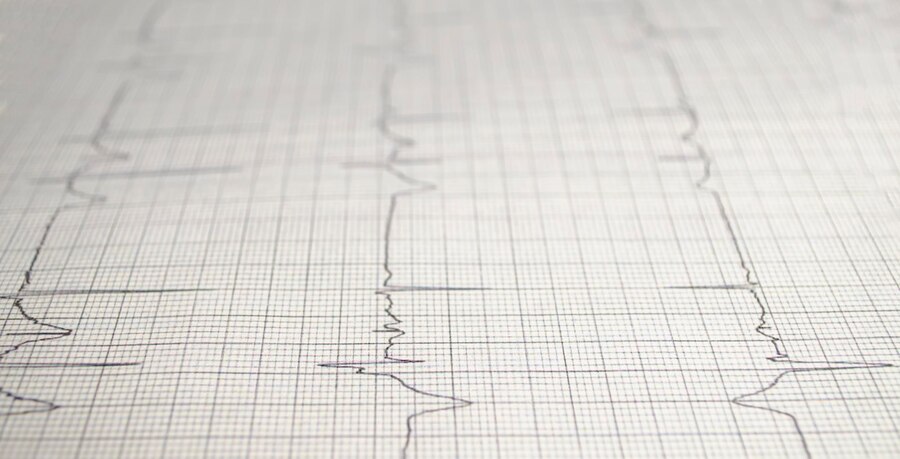
Delta Waves ECG – Understating The Delta Waves Interpretations
The presence of delta waves on an ECG indicates an additional conduit carrying electricity from the atria to the ventricles.
Jun 16, 202288 Shares1.9K Views
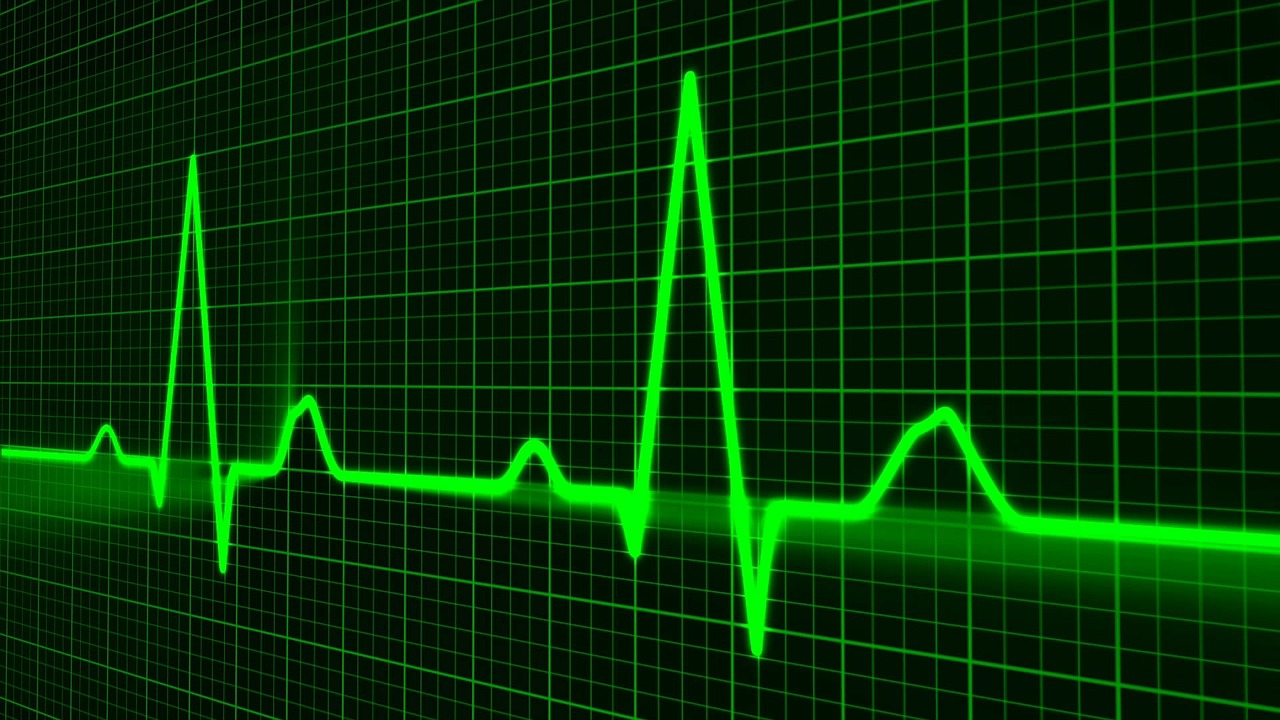
Delta waves ECGindicates that there is an additional channel carrying electricity from the atria to the ventricles.
In the QRS complex, the Delta wave is a slurred upstroke.
It is related to pre-excitation of the ventricles and so frequently results in a shortening of the PR interval.
It is most usually linked to pre-excitation disorders like WPW.
Delta Waves ECG Causes
A delta wave slurs the upstroke of the QRS complex.
Because the action potential from the sinoatrial node may swiftly conduct to the ventricles through the auxiliary channel, the QRS occurs shortly after the P wave, resulting in the delta wave.
When the sinus node generates an action potential in a typical person, it must travel via the AV node to reach the ventricles.
When an auxiliary channel is present, the sinus node action potential might travel via the bypass tract before reaching the AV node, causing the ventricles to depolarize quickly.
This is known as "pre-excitation," resulting in a shorter ECG PR interval.
Delta Waves History
Wolff L, Parkinson J, and White PD publish the eleven cases as the authoritative description of the illness in 1930 – 'Bundle Branch Block with Short P-R Interval in Healthy Young People Prone to Paroxysmal Tachycardia.'
A study of the literature validated and recognized the examples mentioned above.
The broad QRS complex was mistakenly supposed to be created by a form of bundle-branch block, according to Wolff, Parkinson, and White.
1933 – Wolferth and Wood proposed that the abnormal slurring of the initial part of the QRS complex and prolongation of the QRS complex were caused by an actual acceleration of the passage of the impulse from the auricle to a section of the ventricle, consistent with the possibility that an accessory pathway of AV conduction described by Kent between the right auricle and right ventricle could be responsible for the phenomenon manifested.
1944 – Marcel Segers, together with Lequime and Denolin, proposed the to depict the triangular form at the base of the upsloping QRS complex 'deformation of the PQ section is the consequence of an extra electrical deflection that we propose to name', they said.
This was thereafter referred to as the 'delta wave.'
Segers et al., on the other hand, claimed that the wave was a separate and independent wave between P and Q.
They did say that the wave might merge with the base of the QRS complex to generate a slurred upstroke, and they associated the wave fusion with the WPW bundle branch phenomena.
Wolff Parkinson White Syndrome
Wolff-Parkinson-White (WPW) syndrome is a pervasive cardiac disorder in which the heart beats excessively quickly for extended periods.
An additional electrical connection in the heart is the source of the problem.
This cardiac issue is present from birth (congenital), yet symptoms may not appear until later in life.
A large number of cases are diagnosed in otherwise healthy young people.
Sometimes the additional electrical connection does not create symptoms and is only discovered when an electrocardiogram (ECG) is performed for another reason.
Delta Wave ECG Differential Diagnosis
Wolff-Parkinson-White syndrome is characterized by pre-excitation of the cardiac ventricles caused by an auxiliary route known as the Bundle of Kent.
Sudden mortality from WPW syndrome is uncommon (incidence less than 0.6 percent) and is caused by the accessory pathway's influence on tachyarrhythmias in these patients.
The surface ECG in an asymptomatic person is widely used to detect WPW syndrome.
It appears as a delta wave, a slurred upstroke in the QRS complex accompanied by a brief PR interval.
If the patient has atrial fibrillation, the ECG will indicate fast polymorphic wide-complex tachycardia (without turning points).
Wolff-Parkinson-White syndrome is sometimes linked to Leber's hereditary optic neuropathy (LHON), a mitochondrial illness.
Electrical activity begun in the SA node goes down the auxiliary route and the AV node to stimulate the ventricles through both pathways in people with WPW.
This combination of atrial fibrillation with WPW is considered risky, and most antiarrhythmic medications are not recommended.
People Also Ask
What Happens During Delta Waves?
Delta waves in the EEG are high-amplitude brain waves linked with profound sleep periods.
Delta waves are also linked to brain activities other than deep sleep; for example, high frontal delta waves in waking persons are related to cortical plasticity.
What Does Wolff-Parkinson-White Syndrome Look Like On EKG?
WPW syndrome is related to the following classic ECG findings:
- The presence of a brief PR interval (less than 120 ms)
- A large QRS complex that lasts more than 120 ms and has a slurred beginning of the QRS waveform, known as a delta wave, in the early part of the QRS.
Which Disorder Produces A Delta Wave?
Paroxysmal supraventricular tachycardia is the most prevalent type of irregular heartbeat.
Conduction via the supplementary channel produces a delta wave.
An individual with Wolff–Parkinson–White syndrome has a distinctive "delta wave" (arrow).
What Does A Delta Wave Mean On ECG?
The ECG detects the electrical activity in your heart as well as the pace of your heart.
A delta wave on the ECG indicates that there is an additional conduit carrying electricity from the atria to the ventricles.
This extra channel causes the ventricles to function earlier than usual, resulting in the anomaly.
Conclusion
In patients with Wolff-Parkinson-White syndrome, delta waves ECG can be seen.
Electrical activity in the heart is initiated in the sinoatrial node and propagates to the atrioventricular node, then to the heart's ventricles through His bundle.
Wolff-ParkinsonWhite syndrome should be identified on electrocardiograms (ECGs) since it can mimic ischemic heart disease, ventricular hypertrophy, and bundle branch block.

Suleman Shah
Reviewer
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.
Latest Articles
Popular Articles