Aryl Hydrocarbon Receptor - How Does It Affect Chronic Kidney Disease?
The aryl hydrocarbon receptor (AHR) is a basic helix-loop-helix transcription factor that binds to different endogenous and xenobiotic ligands that control its stability, transcriptional activity, and cell signaling. Chronic kidney disease is strongly linked to AHR activity at all stages.
Author:Suleman ShahReviewer:Han JuAug 04, 20220 Shares444 Views
The aryl hydrocarbon receptor(AHR) is a basic helix-loop-helix transcription factor that binds to different endogenous and xenobiotic ligands that control its stability, transcriptional activity, and cell signaling.
Chronic kidney disease is strongly linked to AHR activity at all stages. Many different kinds of organic molecules can bind to and turn on AHR.
These molecules, known as "ligands," are thought to either damage the glomeruli and tubules or protect them from damage.
About 37 million (1 in 7) US adults have chronic kidney disease (CKD), which is the ninth leading cause of death.
It is thought that 13.7 - 15.1% of the nearly eight billion people in the world have CKD, which is more than a billion cases.
Current treatments for CKD can slow or even stop the disease from getting worse, but most patients still get worse.
Fibrosis In Chronic Kidney Disease
Tissue damage caused by injury or illness causes remodeling and repair. When this mechanism isn't working right, it throws off the balance of extracellular matrix (ECM) homeostasis and causes fibrotic tissue.
The main families of molecules in the kidney interstitial ECM include collagen (types I, II, III, V, VI, VII, and XV), glycoproteins (e.g., fibronectin, laminin), proteoglycans (e.g., biglycan, decorin, versican), and glycosaminoglycans (e.g., chondroitin sulfate, dermatan sulfate, heparin sulfate, hyaluronan). These chemicals work together to attach cells inside tissue.
The human genome encodes three TGF-β isoforms (TGF-β1, TGF-β2, TGF-β3). In termsof extracellular matrix biology, all three isoforms have the potential to promote collagen production and tissue fibrosis. Inflammatory cells secrete inactive TGF-β1 that is non-covalently bound to a latency associated peptide (LAP) that is disulfide bound to the latent TGF-β binding protein (LTBP).
Tissue transglutaminase-2 binds the LTBP-released complex:
LAP:TGF-1β is incorporated into the ECM via enzymatic cross-linking of LTBP to fibronectin and possibly other ECM proteins associated with elastic fibers. Active TGF-1β is released from the large latent complex via integrin-mediated mechanical deformation of the ECM and/or protease-mediated degradation of LAP (e.g., MMPs, thrombospondin-1, and plasmin).

Aryl hydrocarbon receptor
Therapies For Chronic Kidney Disease
Several techniques are used to treat CKD. Treatment of the underlying condition, such as diabetes, lupus, vasculitis, or other systemic disorders, may slow or stop the growth.
For example, the sodium-glucose transport protein 2 (SGLT2) inhibitor dapagliflozin was approved for progressive non-diabetic kidney diseaseof many etiologies following studies demonstrating efficacy in lowering the risk of a combined endpoint of kidney function decline, kidney failure, cardiovascular death, and heart failurehospitalization.
Pathway-targeted therapies for primary renal disorders or syndromes are increasingly accessible or in development (e.g., focal segmental glomerulosclerosis, membranous nephropathy, and polycystic kidney disease).
On the other hand, there are about 10,000 rare diseases, and it's not known how many of them have renal symptoms or if they can be treated.
Diet and blood pressure drugs (goal <130/80), antifibrotic therapy (inhibitors of renin, angiotensin II, and aldosterone, the latter being a powerful profibrotic molecule), dietary salt restriction, and thiazide diuretics are among them (the latter potentiates the antiproteinuric effects of the renin-angiotensin-aldosterone system antagonists).
SGLT2 inhibitors slow the course of kidney damage in diabetes, and the same effect has recently been shown in non-diabetic renal disease, potentially through lowering proximal tubule stress.
Aryl Hydrocarbon Receptor In Drug Metabolism
AHR has a pivotal role in regulating the clearance of xenobiotics and particular endogenous compounds (e.g., metabolites of tryptophan, arachidonic acid, and hemoglobin), which also bind and activate AHR during various processes, including development, hematopoiesis, and disease pathogenesis.
In the clearance of these molecules, the AHR:ARNT heterodimer induces the expression of proteins involved in each of the three metabolic biotransformation pathways. These proteins stop molecules inside the cell and outside the cell from doing their jobs and help them leave the cell.
Phase I metabolism includes oxidation, reduction, and hydrolysis of substrates to generate more water-soluble, but generally still active, xenobiotic molecules.
AHR-induced cytochrome P450 enzymes are a common measure of AHR activation in the liver. Their importance in the kidney and the immune systemis still being researched. Cytochrome P450 enzymes oxidize substrates and therefore contribute to phase I metabolism.
Conjugating enzymes add a hydrophilic group to targeted molecules during Phase II metabolism; these protein modifications include glucuronidation, sulfation, acetylation, and methylation. The kidney expresses UDP-glucuronosyltransferase (UGT)-1A5, UTG1A6, UGT1A7, UGT1A9, UGT2B4, UGT2B4, and UGT2B17.AHR can induce UGT1A1 and UGT1A6 in human cell lines.
Phase III metabolism includes ATP-binding cassette (ABC) and solute carrier (SLC) transporters that facilitate xenobiotic efflux.
Exposing rat brain capillaries to the AHR ligand, 2,3,7,8-tetrachlorodibenzo-p-dioxin (TCDD, dioxin), induced production of the ABC transporter, P-glycoprotein, also known as multidrug resistance protein (MRP)-1. P-glycoprotein and additional ABC transporters [e.g., MRP2, MRP4, breast cancer resistance protein (BCRP)] are also induced in dioxin-exposed killifish renal proximal tubules.
We would learn more about how the AHR kidney works if we tested these responses on human kidney cells.
Aryl Hydrocarbon Receptor Function In ADP-Ribosylation
Activated AHR and HIF-1α both boost TCDD-inducible poly(ADP-ribose) polymerase (TIPARP/PARP7/ARTD14) transcription. Poly-ADP-ribose polymerases (PARPs) regulate DNA repair, transcription, and cell signaling by adding a single ADP-ribosyl group (mono-ADP-ribosylation/MARylation) or several groups (poly-ADP-ribosylation/PARylation) to substrates (e.g., protein, DNA, and RNA).
While the functional properties of PARPs are still being studied, TIPARP is unusual in that it may adversely regulate its transcriptional activators (AHR, HIF-1α). TIPARP co-localization of the specific transcription factor seems to be involved in the pathways, as does the recruitment of an E3 ligase for ubiquitin-mediated proteasome destruction of the transcription factor.
In these networks that include both AHR and HIFs, AHR is involved in basic metabolic processes and responses to low oxygen levels. This is true during the development and progression of diseases like chronic kidney disease.
AHR Regulatory Mechanisms In Chronic Kidney Disease Signaling Networks
Hypertension, increasing renal fibrosis, and tissue hypoxia are all symptoms of chronic kidney disease. Increased circulating plasma levels of extracellular nicotinamide phosphoribosyltransferase (eNAMPT/visfatin) and blood levels of kynurenine are biochemical characteristics.
The RAAS, TGF-β1 cell signaling, and metabolism all influence these pathologic processes and biomarkers. The responsibilities of AHR in each of these systems are still being defined.
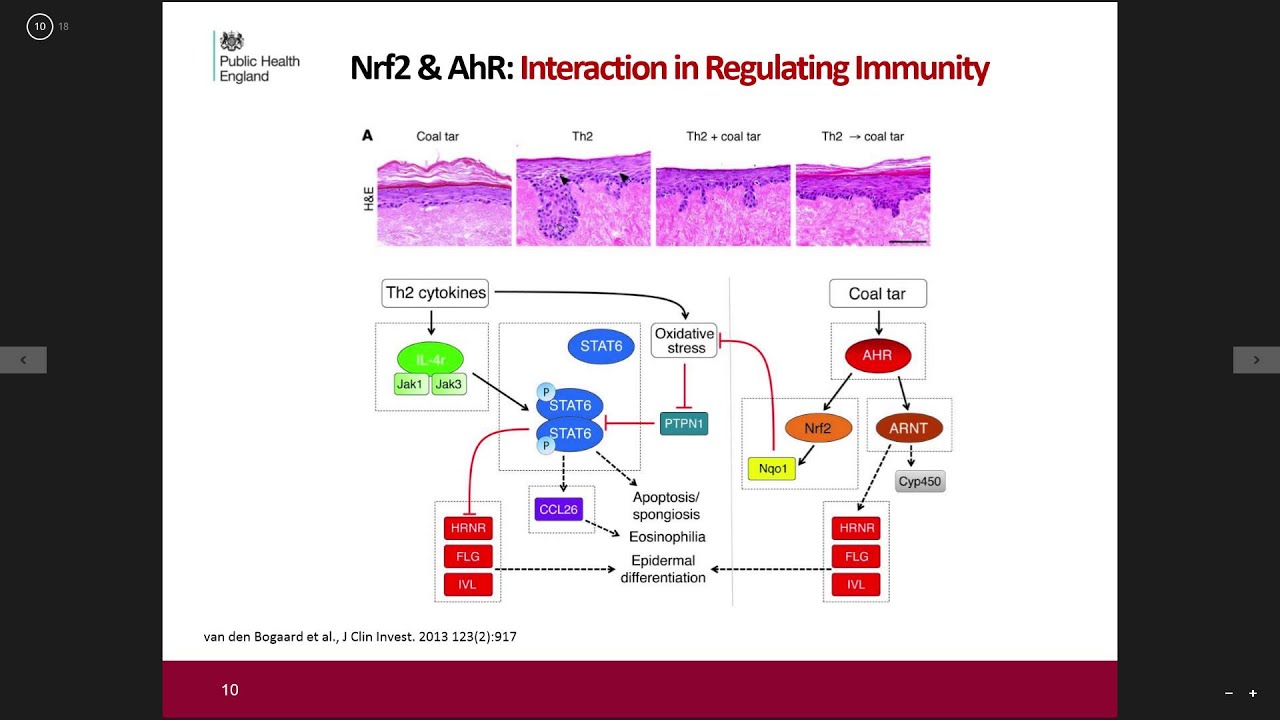
The Aryl Hydrocarbon Receptor: Martin Leonard
Renin–Angiotensin–Aldosterone System (RAAS) And AHR
The RAAS pathway is made up of a series of enzyme activities that help to regulate extracellular fluid volume, arterial pressure, tissue perfusion, electrolyte balance, and wound healing.
Renin is released by glomerular juxtaglomerular cells. It changes angiotensinogen, which is made by the liver, into angiotensin I (Ang I). Angiotensin converting enzyme (ACE) then cuts Ang I into angiotensin II (Ang II).
Binding of Ang II to the Ang II type 1 receptor (AT1R) causes vasoconstriction as well as the synthesis of aldosterone, which stimulates renal tubular salt reabsorption and fibrogenesis.
ACE2 inactivates Ang II by cleaving and digesting Ang I and Ang II into Ang (1-7) that binds the Mas receptor and the AT2R. By doing these things, ACE2 blocks the effects of ACE/Ang II/AT1R activity on blood vessels, inflammation, blood clots, and scar tissue.
The roles of AHR in the RAAS signaling pathways seem to be dependent on the degree of AHR and AHR ligand expression.
AHR-deficient animals develop cardiac hypertrophy through pathways including HIF-1α cell signals, Ang II-induced fibrosis, higher endothelin-1 plasma levels, and increased mean arterial pressures.
Blood pressure stays normal in heterozygous AHR (+/−) mice, and AHR (+/−) animals are more susceptible to ACE inhibition and an endothelin-1 receptor antagonist than AHR (−/−) null mice.
The effects of AHR overexpression on RAAS activity have not been thoroughly studied. AHR overexpression in adipocytes reduces the half-lifeof PPAR-γ by attracting it to the cullin 4b (CUL4B)-RING E3 ubiquitin ligase complex, where it is degraded in the proteasome.
Because decreased PPAR-γ activity stimulates AT1 production and signaling in human fibroblasts, AHR overexpression may also influence the ACE/Ang II/AT1R pathway. AHR may also bind estrogen receptor (ER)-α to the CUL4B-RING E3 ubiquitin ligase complex, resulting in ubiquitination or target TIPARP ADP-ribosylation.
These post-translational changes that increase ER-α proteasome degradation suggest that AHR may play a role in gender disparities in RAAS activity.
Metabolism And Aryl Hydrocarbon Receptor
During the course of CKD, ischemia and oxidative stress produce metabolic stresses (e.g., hypoxia) and the generation of pro-inflammatory mediators (e.g., IL-1β, TNF, IL-6).
Inflammation and metabolism were identified as the two primary pathways in the pathophysiology leading to CKD development in a thorough pathway map analysis of gene sets from 157 European patients with nine distinct forms of CKD.
These responses are regulated by transcription factors such as NFκ-B and HIFs, which interact with AHR.
HIF-α has three isoforms: HIF-1α, HIF-2α, and HIF-3α, which are encoded by different genes: HIF1A, EPAS1, and HIF3A.
HIF-1α and HIF-2α are expressed in the kidney, compete for the dimer partner ARNT with AHR, and may be degraded in either the proteasome or the lysosome.
Oxidative stress, hypoxia, Ang II, and some peptides (for example, human epidermal growth factor receptor-2 (HER-2), IL-1β, and insulin) diminish HIF post-translational changes that target the protein for destruction and hence maintain HIF expression.
The most well-known HIF-1α transcriptional responses include the expression of genes whose products are involved in glycolysis and lactate generation.
The HIF-1α:ARNT heterodimer specifically stimulates transcription of SLC2A1 (Solute Carrier Family two Member 1, GLUT1), HK1 (hexokinase 1), HK2 (hexokinase 2), PFK (phosphofructokinase), ALDOA (aldolase, fructose-bisphosphate A), GAPDH (glyceraldehyde-3-phosphatedehydrogenase (lactate dehydrogenase A).
Anaerobic metabolism reduces nicotinamide adenine dinucleotide (NAD) levels while increasing the synthesis of the reduced form, NADH.
Despite their distinct roles in the RAAS, both AT1R and AT2R may promote HIF-1α stability in response to Ang II. More research is needed to understand the functions of AT1R and AT2R HIF-1α cell signaling in CKD.
The NF-κB Pathway And AHR
Both the conventional and non-canonical NF-B pathways interact with AHR. There are five proteins in the NF-κB transcription factor family: p65 (RelA), RelB, c-Rel, p105/p50 (NF-κB1), and p100/p52 (NF-κB2). As inactive precursors, p105 and p100, NF-κB1 and NF-κB2 are generated.
RelB is also associated with p100. Cell signals cause the inactive precursors to be proteolytically processed, resulting in the functional components p50 and p52. The Rel proteins p65 and c-Rel bind to inhibitory protein kinases (e.g., IκBα, IκBβ and IκBε). Cell signals phosphorylate inhibitory kinases, which tells the kinases to break down and let p65 or c-Rel out.
NF-κB proteins combine to generate transcriptionally active homo and heterodimeric complexes. The p65 transcription factor is most typically associated with p50, although it may also form homodimers and interact with c-Rel and p52. RelB has only been shown to form heterodimers with p50 or p52.
The conventional route includes p65/p50 activation, while the non-canonical pathway involves RelB activation. In mouse embryonic fibroblasts, p65 and RelB have negative crosstalk, and RelB reduces TNF production in mouse renal fibroblasts, which is a common mediator in CKD.
People Also Ask
Where Is The Aryl Hydrocarbon Receptor?
Protein domains are discovered in the aryl hydrocarbon receptor (AHR) and the nuclear translocator of the aryl hydrocarbon receptor (AHRNT) (ARNT). The basic helix-loop-helix (bHLH) region contains the nuclear localization sequence (NLS) and nuclear export sequence (NES). The bHLH is also important in DNA binding.
What Are Aryl Hydrocarbon Receptor Ligands?
The aryl hydrocarbon receptor (AHR) is a ligand-dependent transcriptional factor that can recognize a diverse variety of external and endogenous chemicals. AHR ligands have different shapes, and the way they bind to mouse and human AHR may be very different.
Where Is Aryl Hydrocarbon Receptor Expressed?
Aryl hydrocarbon receptor is expressed in barrier tissues (e.g., the gut, the skin, and the lung) by both immune cells like lymphocytes and tissue-structuring cells like epithelial and stromal cells, as well as in the liver by hepatocytes, consistent with its function as an environmental sensor.
What Is The Connection Of The Aryl Hydrocarbon Receptor (AHR) And Dioxin?
The dioxin/aryl hydrocarbon receptor (AHR) is a ligand-activated transcription factor that regulates the transcription of a number of genes that encode xenobiotic metabolizing enzymes. Environmental contaminants such as polycyclic aromatic hydrocarbons and polychlorinated dioxins are known as receptor ligands.
Conclusion
The aryl hydrocarbon receptor is a pleiotropic cell signaling protein that has a variety of ligand-specific activities.
The increased quantities of uremic solutes that serve as aryl hydrocarbon receptor ligands as chronic kidney disease progresses underscore the importance of aryl hydrocarbon receptor activation in these disorders.
The aryl hydrocarbon receptor aids in the biotransformation of molecules during xenobiotic clearance, and these activities merit additional investigation in renal pathology.
Aryl hydrocarbon receptor competition with HIF-1α for binding to ARNT in pro-inflammatory and anaerobic responses, as well as AHR antagonism of TGF-β1 cell signaling in fibrogenesis, support AHR targeting to slow the evolution of chronic kidney disease.
AHR increases RNA expression and protein production of the rate-limiting enzyme, IDO1, in the NAD de novo biosynthesis pathway and binds compounds along this route that accumulate in chronic kidney disease.
TIPARP activity requires NAD, which is required for the recruitment of an E3 ligase for ubiquitin-mediated proteasome degradation of AHR. It's likely that kynurenine and NAMPT leak out of cells and into the bloodstream, rather than being broken down into NAD by metabolism inside cells.
Further research into AHR-mediated ACE2 regulation and the downstream effects of the ACE2 cleavage product, Ang-(1-7), on Mas and AT2R may lead to the identification of new therapeutic targets in hypertension and fibrosis. Because each of these AHR activities may be influenced by crosstalk with ER-α, PPAR-γ, or NF-κB subunits, a more precise evaluation of HSP90 binding affinity and availability in various cell signaling pathways during CKD is required.
Jump to
Fibrosis In Chronic Kidney Disease
Therapies For Chronic Kidney Disease
Aryl Hydrocarbon Receptor In Drug Metabolism
Aryl Hydrocarbon Receptor Function In ADP-Ribosylation
AHR Regulatory Mechanisms In Chronic Kidney Disease Signaling Networks
Renin–Angiotensin–Aldosterone System (RAAS) And AHR
Metabolism And Aryl Hydrocarbon Receptor
The NF-κB Pathway And AHR
People Also Ask
Conclusion

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles